Artificial sweeteners were meant to be a hack – a shortcut to sweetness without the metabolic chaos of sugar. However, by trying to outsmart nature, we may have triggered a new layer of biological confusion. These chemicals – often 200-500 times sweeter than table sugar, are now embedded in the modern diet. From morning protein shakes to the “zero calorie” desserts, they’re everywhere!
Why are they taking over the market? Less sugar, fewer calories, better glycaemic control. More people are making the switch from table sugar to artificial sweeteners. But the real question is: is this a well-informed switch? And are people truly aware of its consequences?
What are artificial sweeteners, really?
Artificial sweeteners are lab engineered molecules designed to mimic the taste of sugar – hundreds of times sweeter, but with little to no caloric value. They are not sugar. They are sugar mimics.
They do not nourish the body. They stimulate it – interacting with our systems in ways science is only beginning to decode.
They fall into two categories:
- Nutritive sweeteners: These resemble sugar and carry some caloric content.
- Non-nutritive sweeteners: These include compounds like sucralose, saccharin, and acesulfame potassium (Acesulfame-K). They are meant to be ultra sweet, calorie free, and shelf stable.
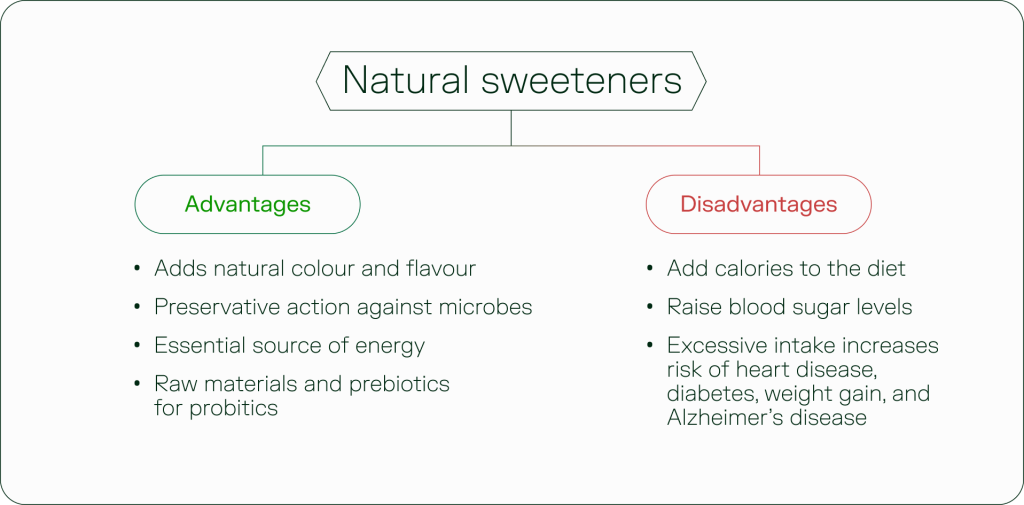
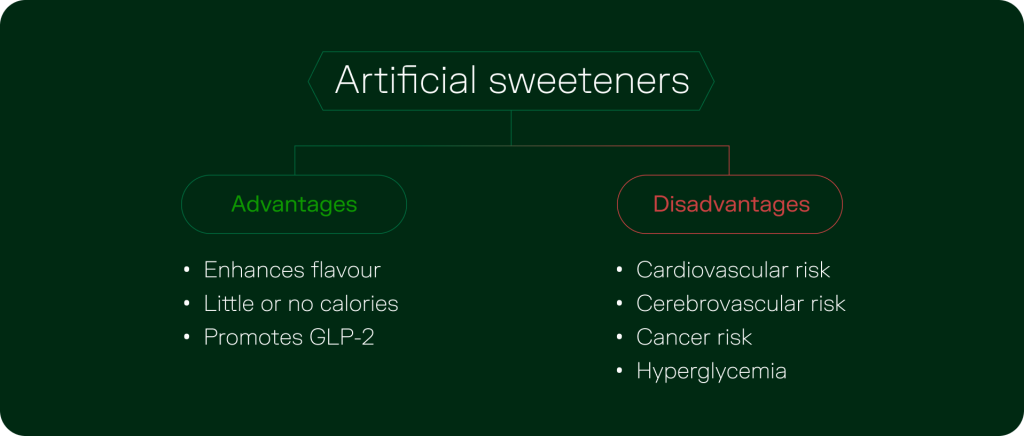


Taste drives choice. It is one of the most powerful forces shaping how we eat – and why we overeat. In a landscape filled with ultra processed foods; it’s increasingly devoid of real ingredients, and sweetness is now a proxy for pleasure. When sugars are removed, something needs to fill that gap.
Artificial sweeteners in diabetes and weight management
The main pitch behind artificial sweeteners is simple: same sweet taste but not as harmful. That’s why they’ve become so common in diabetes care and weight loss products.
Certain artificial sweeteners are not true carbohydrates. Since they are much sweeter than natural sugars, you need less of them to get the same effect. Unlike natural sugars – they don’t get fully absorbed by the body; some are excreted unchanged. In theory, this means no glucose spike, no insulin surge. That’s a win for anyone trying to manage blood sugar.
Artificial sweeteners are also marketed as a weight loss ally – helping cut down daily calorie intake.
But, why are artificial sweeteners harmful?
Some short term studies suggest that artificial sweeteners may help manage diabetes and obesity. But that is far from the full picture. Take saccharin – one of the earliest artificial sweeteners. Discovered by accident, it was later banned over cancer concerns and then reinstated after regulatory reviews. It remains in use today. That history alone should prompt questions about its long-term safety.
More critically, the widespread use of artificial sweeteners, especially in ultra processed foods – is now linked to the very conditions they were meant to prevent. Multiple studies report a positive association between regular artificial sweetener consumption and an increased risk of type 2 diabetes.
So while these compounds were introduced as solutions, they may be quietly contributing to the problem.
How do artificial sweeteners disrupt metabolism?
Artificial sweeteners don’t pass through the body unnoticed. They impact gut health, and by extension – metabolism. With consistent use, the beneficial bacteria-lactobacillus and bifidobacterium declines and the growth of harmful bacterial growth increases. These compounds alter the balance of gut bacteria.
This microbial imbalance – known as dysbiosis, disrupts gut diversity and reduces the production of short-chain fatty acids (SCFAs). SCFAs play a critical role in how we metabolise glucose and fats.
The downstream effects? Glucose intolerance raised triglyceride levels, systemic inflammation, insulin resistance, and eventually, increased risk for obesity, type 2 diabetes, hypertension, and cardiovascular disease.
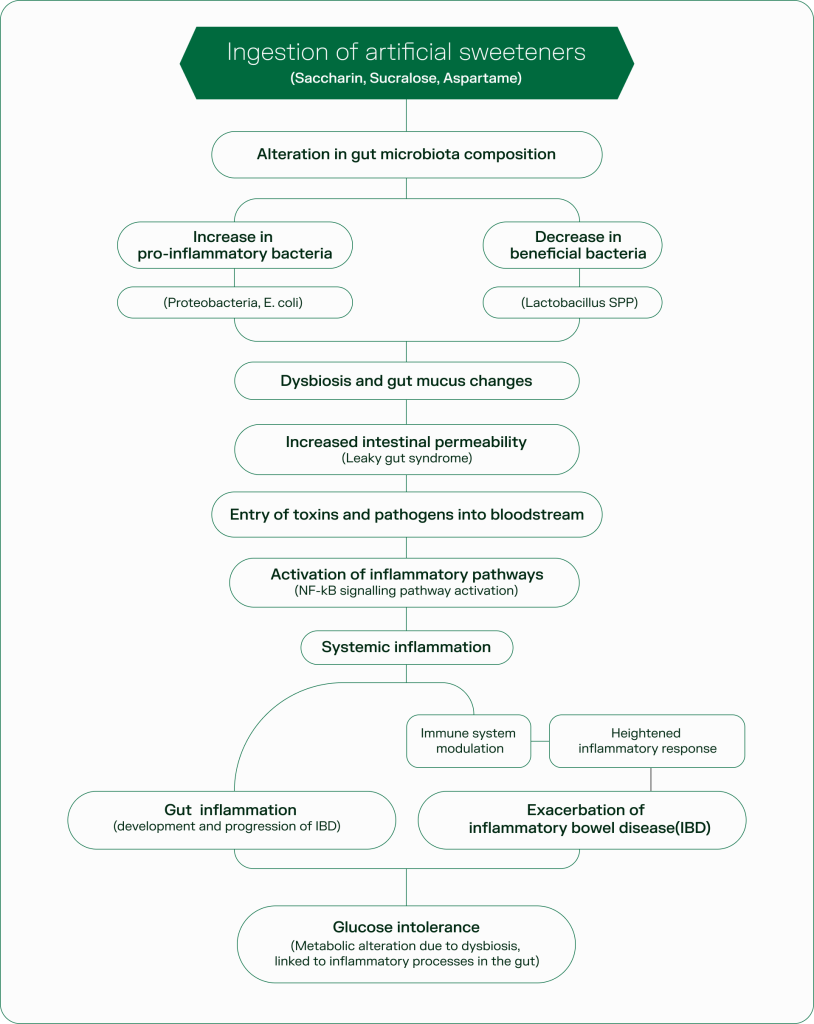
Inflammation and the leaky gut
When the gut microbiome is disrupted, the gut lining weakens. Beneficial bacteria maintain this barrier by producing short-chain fatty acids (SCFA’s). But when these microbes decline, gut integrity starts to break down.
Harmful bacteria begin to dominate, releasing toxic metabolites like lipopolysaccharides (LPS). These can slip through the gut wall – a condition often referred to as “leaky gut.” Once in the bloodstream, these toxins trigger a chronic immune response, fuelling systemic inflammation and development of diabetes.
Glucose intolerance
The body doesn’t wait for food to hit the gut to start reacting. Insulin release is triggered by the sight, smell, or taste of food; this is called the cephalic phase response.
Acesulfame-K takes advantage of that. It delivers intense sweetness without any calories. But that’s exactly the problem. The body gets the signal – sweet taste – so it releases insulin. But there’s no actual glucose to process.
The mismatch creates confusion. Insulin spikes without a purpose. Over time, that constant overstimulation can dull insulin receptors, increasing the risk of insulin resistance.
For people with diabetes or prediabetes, this becomes even more important. Artificial sweeteners might not be helpful – they may be nudging the system in the wrong direction.
Obesity
One of the more counterintuitive findings? Artificial sweeteners are associated with higher rates of obesity.
When sweet taste isn’t paired with actual energy, the brain struggles to regulate appetite. Hunger and satiety signals become unreliable. People end up eating more.
At the same time, artificial sweeteners disrupt the gut microbiome – shifting it toward a profile commonly observed in obesity: reduced microbial diversity, decreased short-chain fatty acid (SCFA) production, and increased levels of pro-inflammatory metabolites like lipopolysaccharides (LPS).
There’s also evidence that these compounds directly impair gut immune defences – triggering low-grade inflammation that alters how the body stores fat and uses energy.
Neurodegeneration
Aspartame, sucralose, and saccharin are linked to increased oxidative stress and neuroinflammation. They can disrupt the blood-brain barrier and affect cerebral blood flow – both of which accelerate cognitive decline.
The gut-brain axis plays a role here too. When the gut microbiome is compromised, it sends inflammatory signals that worsen neurocognitive function. In people with type 2 diabetes or obesity, the neurological impact of sweeteners can be even more severe – contributing to impaired cognition and higher risk of neurodegenerative diseases.
Cancer
Aspartame and acesulfame-K have been associated with a higher risk of cancer – especially obesity related cancers. The carcinogenicity arises because of its ability to cause inflammation, angiogenesis, DNA damage promotion and its ability to inhibit cell death. Saccharin, sucralose, and aspartame also contribute to gut dysbiosis and glucose intolerance – both of which may play a role in cancer development.
Comparing sweeteners: from taste to gut disruption

The real cost of sweetness
Artificial sweeteners promise a simple trade off: sweetness without the sugar. But the hidden cost plays out deep in the body – disrupting gut bacteria, dulling insulin sensitivity, and driving inflammation.
These aren’t just minor side effects. They affect how we age, how we store energy, and how resilient our systems stay over time.
Longevity isn’t about swapping one shortcut for another. It’s about protecting metabolic function at its root – by making food choices that support, not confuse, the body’s natural signals.





